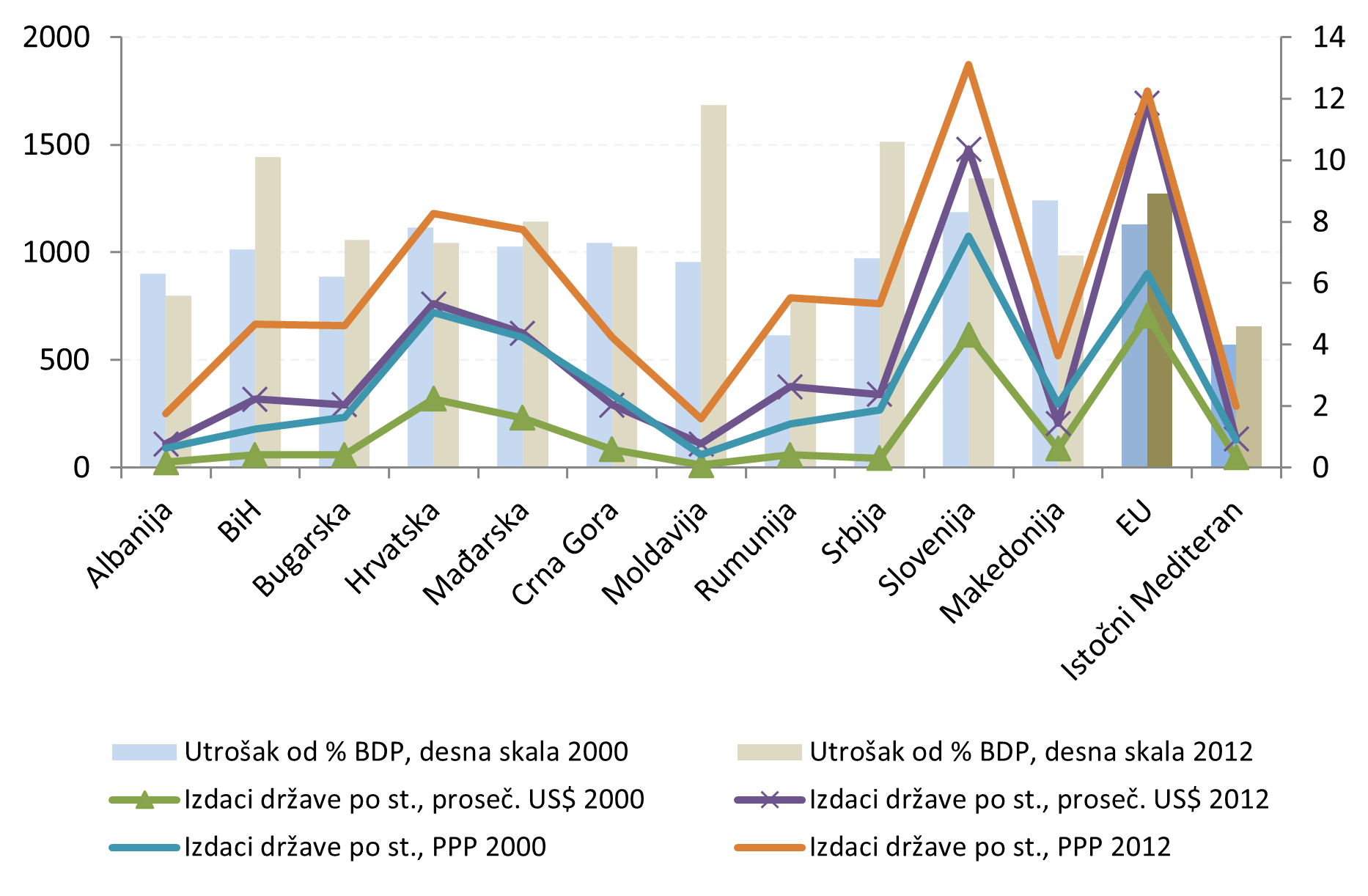
Prema podacima SZO o izdvajanjima za zdravstvenu zaštitu kao procenata BDP-a, Republika Srbija je iznad proseka Evropske unije. Međutim, u poređenju sa drugim evropskim zemljama, Srbija izdvaja u apsolutnom iznosu MALA sredstva za zdravstvenu zaštitu, što je posledica relativno NISKOG nivoa BDP-a Srbije.
Naš sistem finansiranja zdravstvene zaštite je godinama neefikasan. I pored visokog izdvajanja za zdravstvenu zaštitu iz BDP-a, sistem ne uspeva da obezbedi stepen zdravstvene zaštite koji odgovara tako visokom učešću u BDP-u. Činjenica je da stepen razvijenosti zemlje određuje karakter i kvalitet zdravstvene zaštite svake zemlje, ali efikasnost sistema je nešto sasvim drugo. Stoga, važno je pitanje kako sa raspoloživim, a oskudnim, resursima i kapacitetima postići što viši, očekivani, stepen zdravstvene zaštite.
Svaki vid finansiranja, pa i zdravlja, prate asimetrične informacije, i to dominantno moralni hazard. U Srbiji osiguranici uplaćuju sredstva u JEDAN JEDINI republički fond bez mogućnosti nametanja ikakve discipline fondu. Otuda su menadžeri spremniji da se upuste u rizične poduhvate. Razvojem privrede bićemo u prilici da koristimo i dodatne izvore finansiranja, za to su potrebni sposobni menadžeri i adekvatna ogranizcija i upravljanje sistemom. Pri tome, nužno je dostići odgovarajući stepen autonomije menadžmenta u zdravstvu kako bi se izbegao principal-agent problema. Menadžere moraju odlikovati višestruke veštine: planiranje i podela poslova, kontrola rada, pisanje izveštaja, javni nastup i pregovaranje, saradnja sa drugim institucijama, adekvatna realokacija resursa, procena troškova, analiza ekonomske isplativosti, upotreba opreme…
Prema podacima, Srbija za finansiranje zdravstva u velikom procentu izdvaja iz BDP-a, ali prema apsolutnom iznosu to je veoma malo. Kroz ionako niska ulaganja po stanovniku, ouočavamo da odstupanje prosečnog kursa od PPP pokazuje da je nacionalna valuta precenjena. Na približnom nivou su Crna Gora i Bosna i Hercegovina, pa i Makedonija. U relativnom izrazu sve su približne proseku EU, ali daleko od novčanog iznosa po stanovniku u EU.
Svetska zdravstvena organizacija u svom izveštaju navodi da loše zdravlje posledica nejednakosti u redistribuciji ekonomske moći, naglašenih socijalnih nejednakosti, neuravnoteženih prihoda, nedostatka kvalitetnih roba i usluga, čak i na globalnom planu. Nerado se prihvata kolektivno plaćanje subvencionisanje troškova zdravstvene zaštite, pa siromašnije zemlje EU sve više izbegavaju uplate doprinosa. Kod ovih zemalja HITNOST u finansiranju dominira u odnosu na PRIORITETE. Otuda problemi!!! Razvijene zemlje stvaraju nove fondove. Nemačka je 2012. godine uvela novi Fond koji prati redovne naplate doprinosa (77% učestvuje država). Slično je u Irskoj (79% učestvuje država). Holandija ima najsavršeniji model finansiranja kroz nekoliko kanala: za redovne (kratkoročne) tretmane postoji obavezno osiguranje preko privatnih kompanija sa 27%, porezi čine 14%, plaćanje iz džepa građama (OOP) je 9%, dok su dodatni paketi osiguranja 4% i drugi izvori 4%. Prema SZO, najbolje zdravstvene usluge daju Francuzi (77% čine vladine agencije). Sistem zdravstvene zaštite je različit od zemlje do zemlje, dok je u SAD decentralizovan, zasnovan na tržištu i konkurenciji, u EU je na blagostanju orijentisani sistem, a u JIE centralizovan i birokratizovan.
Glavni nedostatak u Srbiji je odsustvo sektorske strategije u zdravstvu.
Ključna rešenja za finansiranje sistema zdravstvene zaštite:
- Adekvatna regulativa ( sa potenciranjem na javno-privatno partnerstvo i zajednička ulaganja),
- Odgovorno upravljanje i odlučivanje (transaprentno i javno dostupno),
- Podsticajna (aktivna) poreska politika.
Izvor: SZO, 2015
According to data from the World Health Organization (WHO) on healthcare expenditure as a percentage of GDP, the Republic of Serbia is above the European Union average. However, compared to other European countries, Serbia allocates SMALL amounts in absolute terms to healthcare, which is a consequence of its relatively LOW GDP level.
Serbia’s healthcare financing system has been inefficient for years. Despite a high share of GDP allocated to healthcare, the system fails to provide a level of healthcare services consistent with such a high percentage of GDP. While the level of economic development determines the character and quality of healthcare in each country, system efficiency is a different matter. Therefore, the key question is how to achieve the highest possible and expected level of healthcare with limited available resources and capacities.
All forms of financing, including healthcare financing, are characterized by asymmetric information, predominantly moral hazard. In Serbia, insured individuals pay contributions into a single national fund without the possibility of imposing effective discipline on the fund. Consequently, managers may be more inclined to engage in risky ventures. With economic development, additional sources of financing could be utilized; however, this requires capable managers, appropriate organization, and effective system governance. It is also essential to ensure a sufficient degree of managerial autonomy in healthcare to avoid the principal–agent problem. Healthcare managers must possess multiple skills: planning and task allocation, supervision, report writing, public speaking and negotiation, cooperation with other institutions, adequate resource reallocation, cost assessment, economic efficiency analysis, and effective use of equipment.
Although Serbia allocates a relatively high percentage of GDP to healthcare, the absolute amount remains very low. Given the already low per capita healthcare expenditure, deviations of the exchange rate from purchasing power parity (PPP) indicate that the national currency is overvalued. Montenegro, Bosnia and Herzegovina, and North Macedonia are at a similar level. In relative terms, these countries are close to the EU average, but they remain far below the EU’s per capita healthcare spending.
The World Health Organization states in its report that poor health outcomes are the result of inequalities in the redistribution of economic power, pronounced social inequalities, income disparities, and a lack of quality goods and services, even on a global scale. Collective payment and subsidization of healthcare costs are often reluctantly accepted, and poorer EU countries increasingly avoid contribution payments. In these countries, URGENCY in financing prevails over PRIORITIES – hence the problems.
Developed countries have established new healthcare funds. Germany introduced a new fund in 2012 to monitor regular contribution payments (with the state participating at 77%). A similar model exists in Ireland (state participation of 79%). The Netherlands has one of the most advanced financing models, operating through multiple channels: mandatory insurance through private companies (27%), taxes (14%), out-of-pocket payments (9%), additional insurance packages (4%), and other sources (4%). According to the WHO, France provides the best healthcare services (77% financed by government agencies). Healthcare systems differ from country to country: in the United States, the system is decentralized and market-based; in the EU, it is welfare-oriented; while in Southeast Europe, it is centralized and bureaucratic.
The main shortcoming in Serbia is the absence of a sectoral healthcare strategy.
Key solutions for healthcare financing:
- Adequate regulation (with emphasis on public–private partnerships and joint investments)
- Responsible governance and decision-making (transparent and publicly accessible)
- Incentive-based (active) tax policy
Source: WHO, 2015